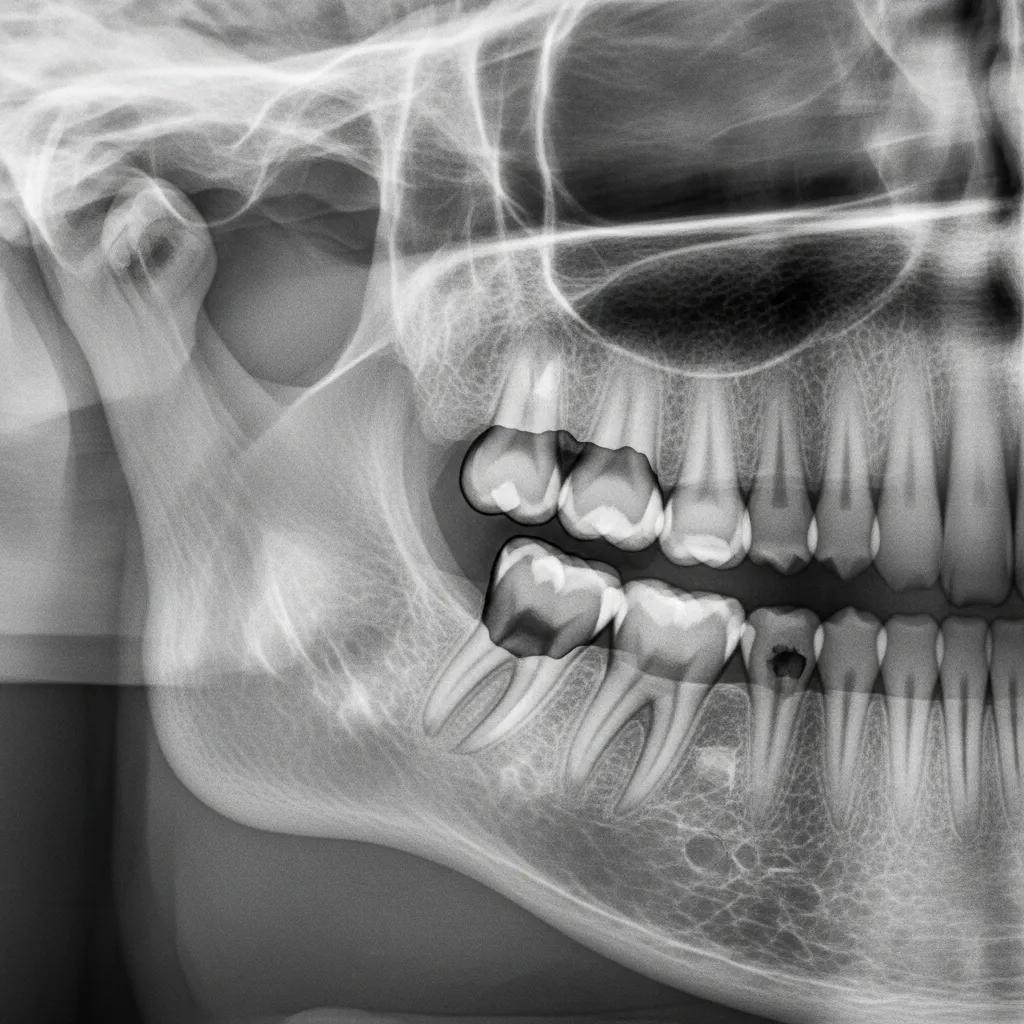
What Causes Tooth Impaction and How to Identify Symptoms

Tooth impaction occurs when a tooth fails to fully erupt into its expected position in the dental arch, and this guide explains why that happens, how to spot signs, and what to do next. Recent clinical reviews indicate that impacted third molars (wisdom teeth) are among the most common eruption disorders, affecting a significant portion of adolescents and young adults; understanding prevalence helps prioritize timely evaluation. This article teaches how impaction develops from space limitations, developmental anomalies, or local pathology, describes characteristic symptoms such as localized pain and swelling, and outlines diagnostic steps clinicians use today. Readers will learn to differentiate impacted wisdom teeth from other impactions, recognize urgent warning signs, and weigh common treatment choices including observation, orthodontic exposure, and extraction. The guide closes with practical pain-management tips and clear indications for seeking professional care so you can move from symptom recognition to effective treatment planning.
What Is Tooth Impaction and Which Teeth Are Commonly Affected?
Tooth impaction is defined as failure of a tooth to erupt fully into the dental arch within the expected developmental window, usually because of mechanical obstruction, inadequate space, or abnormal angulation. This eruption disorder can produce symptoms ranging from asymptomatic radiographic findings to recurrent infection and damage to adjacent teeth, so recognizing impacted teeth early reduces complication risk. Commonly affected teeth include third molars and maxillary canines, though premolars and retained primary teeth may also be involved; prevalence varies with age and genetics. Understanding which teeth are at risk helps clinicians prioritize monitoring and early intervention to preserve oral function and alignment.
How Do Impacted Wisdom Teeth Differ from Other Impacted Teeth?
Impacted wisdom teeth typically erupt later than other permanent teeth and often encounter limited posterior arch space, making them the most frequently impacted tooth type. Their late eruption timing combined with jaw-size mismatch leads to common complications such as pericoronitis, caries on adjacent second molars, and localized swelling that can refer pain to the ear or throat. Because wisdom teeth are posterior and often partially covered by gum tissue, they more commonly present as partially impacted teeth with a higher risk of soft-tissue infection compared with fully impacted anterior teeth. Recognizing these differences clarifies why treatment urgency often differs: some anterior impactions (like canines) are managed predictably with orthodontic exposure, while many wisdom teeth require extraction to prevent recurrent problems.
Indeed, research consistently highlights the prevalence of wisdom tooth impaction and the common necessity of their surgical removal.
Wisdom Teeth Impaction: Prevalence and Surgical Removal
Third molars (M3) are the most commonly impacted teeth, and their surgical removal is one of the most frequent procedures performed by oral and maxillofacial surgeons. The extraction of the impacted third molar is a common treatment.
An insight into acute pericoronitis and the need for an evidence-based standard of care, S Young, 2019
What Are the Types of Tooth Impaction?
Tooth impaction is classified by eruption angle and extent of eruption: vertical, mesioangular, distoangular, and horizontal describe angular relationships, while partial versus full indicates how much of the crown has penetrated tissue. Each meronym—mesioangular impaction, horizontal impaction, vertical impaction, distoangular impaction—describes specific anatomical orientations that influence surgical complexity and risk to adjacent structures. For example, mesioangular and horizontal impactions often increase extraction difficulty and raise the chance of damaging neighboring teeth, whereas vertical impactions may be simpler if space allows. Clinicians use these classifications to plan imaging, surgical approach, and counsel patients on expected recovery and complication risk.
What Causes Impacted Teeth? Understanding the Main Factors
Impacted teeth arise from a combination of developmental, anatomical, and pathological factors that obstruct normal eruption paths or leave insufficient arch space. Key drivers include dental crowding and jaw-size mismatch, genetic predisposition affecting dental development, and local blockages such as cysts, dense bone, or thick overlying gum tissue that physically impede eruption. These causes interact: for instance, a genetically narrow jaw may predispose a patient to crowding that prevents third molars from erupting, while a dental follicle cyst can create localized mass effect that stops a tooth from advancing. Recognizing the root cause guides whether treatment should be preventive (orthodontic), surgical, or observational.
Primary causes of tooth impaction include:
- Dental crowding limiting space for eruption.
- Genetic factors influencing tooth size, number, or jaw development.
- Localized pathologies such as cysts or retained primary teeth.
These main causes often coexist, so a combined management strategy frequently produces the best outcomes.
How Does Dental Crowding and Genetics Lead to Tooth Impaction?
Dental crowding results when the tooth-bearing arch length is insufficient for all permanent teeth, forcing erupting teeth to deviate from their normal path or remain unerupted. Genetics plays a strong role: family patterns of small jaws or large tooth size predict higher impaction risk because inherited jaw dimensions determine available space for eruption. Mechanically, an erupting tooth follows a programmed eruption path; if that path is constricted by adjacent teeth or bone, the tooth becomes malpositioned or trapped. Early orthodontic evaluation can identify crowding risks and, in some cases, preventive expansion or tooth extractions can reduce the chance of future impaction.
What Role Do Cysts, Bone Density, and Gum Tissue Thickness Play?
Localized pathology such as follicular cysts can form around the crown of an unerupted tooth and physically block eruption, often requiring surgical removal before normal eruption can proceed. High bone density or excessive cortical bone can create a rigid barrier to eruption, particularly in adults whose bone remodeling is slower, while thick or fibrous gum tissue may form a soft-tissue impaction that prevents the tooth from breaching the mucosa. Clinically, unexplained delayed eruption, radiographic radiolucencies, or a bulging tissue mass should prompt imaging to rule out cysts or other anatomic obstructions that necessitate surgical management.
What Are the Signs and Symptoms of Impacted Teeth?
Impacted teeth can present with a range of local and regional symptoms that vary by tooth type, impaction depth, and whether infection or cystic change is present. Typical local signs include pain at the site, gum tenderness, redness, swelling, and recurrent pericoronitis around partially erupted teeth, while regional symptoms may include bad breath, difficulty chewing, jaw pain, and even headaches from referred pain. Systemic signs such as fever can appear if an acute infection develops; combinations of persistent pain, swelling, and drainage usually indicate the need for urgent clinical evaluation. Early symptom recognition helps prevent progression to complications like cyst formation or damage to neighboring teeth.
Common symptoms of impacted teeth include:
- Pain or throbbing near an unerupted tooth.
- Swollen, red, or tender gum tissue around the eruption site.
- Persistent bad breath or unpleasant taste associated with drainage.
Recognizing a cluster of these findings—especially pain plus swelling or drainage—warrants prompt dental assessment to avoid worsening infection or structural damage.
SymptomProbable CauseWhat It MeansLocalized posterior swelling and gum rednessPartially impacted wisdom toothSoft-tissue impaction with risk of pericoronitisDelayed eruption of upper canine with palatal bulgeImpacted canineEctopic canine possibly requiring surgical exposureReferred ear or throat pain without oral sourcePosterior molar impactionNerve referral from impacted third molarChronic bad breath or persistent drainageInfection around impacted toothOngoing infection or abscess formation
How Can You Recognize Impacted Wisdom Tooth Symptoms?
Impacted wisdom teeth often present with posterior jaw pain that may radiate to the ear or throat, accompanied by localized gum swelling and difficulty opening the mouth in severe cases. Pericoronitis—the inflammation of gum tissue over a partially erupted wisdom tooth—produces tender, erythematous gingiva and can lead to pus drainage and foul taste if infected. Patients frequently report episodic flare-ups that improve with home care but recur, signaling that definitive dental evaluation is needed. When symptoms include fever, spreading swelling, or difficulty breathing or swallowing, immediate professional care is required.
Understanding the specific characteristics of pericoronitis is crucial, as it is a common complication directly linked to impacted wisdom teeth.
Pericoronitis: Symptoms, Treatment, and Impacted Wisdom Teeth
Pericoronitis is an infection associated with impacted lower third molars that can necessitate the removal of these teeth. The clinical features of this condition are described and its treatment outlined, including the use of antibiotics and local debridement.
Pericoronitis: treatment and a clinical dilemma, 2009
What Are the Signs of an Impacted Canine Tooth?
Impacted canines commonly reveal themselves as a missing tooth in the dental arch after the normal eruption window, sometimes with a palpable bulge on the palate or along the gum where the tooth is trapped. Because canines play a critical role in smile aesthetics and occlusion, their impaction often produces spacing problems, midline shifts, or compromised bite development that are best managed with combined orthodontic and surgical planning. Clinical clues include prolonged absence of the tooth on radiographs, asymmetric eruption patterns, and space discrepancy in the arch. Early detection—often during adolescence—permits interventions that can guide the canine into the arch and minimize invasive surgery.
How Is Tooth Impaction Diagnosed?
Diagnosis of tooth impaction relies on a careful dental history, focused clinical examination, and targeted imaging to determine tooth position, orientation, and relationship to adjacent anatomy. The clinical exam looks for eruption gaps, soft-tissue bulging, signs of infection, and palpation findings, while imaging options—periapical x-rays, panoramic radiography, and cone-beam computed tomography (CBCT)—provide increasingly detailed localization. Together, history, exam, and imaging form a semantic triple: Tooth (entity) → exhibits (relationship) → delayed eruption or malposition (entity), which guides treatment planning. Timely diagnosis distinguishes between conservative monitoring and the need for surgical or orthodontic intervention.
Diagnostic ToolTypical FindingClinical UsePeriapical x-rayLocalized tooth position, adjacent root statusInitial assessment of tooth and nearby structuresPanoramic x-rayOverall dental arch, third molar angulationScreening for impaction patterns and jaw relationshipsCBCT (3D)Precise 3D localization, proximity to nervesSurgical planning for complex impactionsClinical examSoft-tissue status, eruption gapsDetermines urgency and guides imaging selection
After a diagnostic workup, many patients benefit from local clinics equipped to perform both imaging and subsequent treatment planning. Bespoke Dental in Lutz, Florida offers comprehensive clinical exams and standard radiographic assessments, with advanced imaging available when three-dimensional localization or surgical planning is required. The practice's focus on wisdom teeth care and services such as extractions and jaw surgery for complex impactions supports a coordinated approach: diagnosis leads directly to a customized plan, and patients can schedule a consultation to review imaging and treatment options with experienced clinicians.
What Diagnostic Tools Do Dentists Use for Impacted Teeth?
Periapical and panoramic x-rays are standard first-line imaging that reveal tooth position, angulation, and relationships to adjacent teeth, and they are sufficient for many routine impaction assessments. CBCT provides three-dimensional detail of root morphology, proximity to the inferior alveolar nerve, and bone volume, making it essential for complex surgical planning or evaluating impacted canines prior to orthodontic exposure. Clinicians also use clinical probes and vitality testing on adjacent teeth to check for pulpal status when impaction threatens neighboring roots. Selecting the appropriate diagnostic sequence minimizes risk and improves surgical planning accuracy.
Beyond its diagnostic precision, studies also suggest that the use of advanced imaging like CBCT can significantly reduce patient anxiety regarding upcoming wisdom tooth surgery.
CBCT for Wisdom Tooth Impaction Diagnosis & Anxiety Reduction
This cross-sectional study explored the psychosocial impact on patients undergoing wisdom tooth surgery of the current evidence-based recommendation to only undertake additional cone-beam computed tomography after panoramic X-ray shows a high risk of nerve injury. The study included a total of 119 participants, where having a CBCT resulted in a self-reported 31% reduction in anxiety about the upcoming wisdom tooth surgery.
Cone-Beam Computed Tomography in Wisdom Tooth Surgery Can Aid Informed Decision-Making and Reduce Presurgical Anxiety, K Khalaf, 2025
When Should You See a Dentist in Lutz, FL for Suspected Impaction?
Seek dental evaluation when you experience persistent pain, swelling, recurrent infections around a partially erupted tooth, visible asymmetry in eruption, or unexplained delayed tooth emergence past normal age ranges. At the first appointment you can expect a focused history, clinical examination, and appropriate imaging to confirm impaction type and develop a treatment plan; this may include monitoring, referral for orthodontic consultation, or surgical removal. Prompt evaluation prevents progression to complications such as cysts, infection, or damage to adjacent teeth. For local patients, a timely visit to a nearby practice ensures coordinated imaging and management by clinicians experienced in wisdom teeth care and surgical extraction.
What Are the Treatment Options for Impacted Teeth?
Treatment options span conservative monitoring, orthodontic-surgical exposure with traction (often for canines), surgical extraction (simple or complex), and in rare severe cases, jaw surgery to correct anatomic limitations. Choosing among observation, orthodontics, and surgery depends on symptoms, risk to adjacent teeth, patient age, and the specific impaction type. Conservative observation is appropriate for asymptomatic, fully covered impactions without pathology, whereas symptomatic or damaging impactions typically require extraction or surgical exposure with orthodontic guidance. Treatment selection balances short-term recovery, long-term function, and risk of complications.
- Observation and periodic radiographic monitoring for asymptomatic, low-risk impactions.
- Orthodontic exposure and traction for impacted canines that can be guided into the arch.
- Surgical extraction for symptomatic wisdom teeth, cystic change, or damage to adjacent teeth.
These options are chosen after diagnostic assessment to align with patient goals and clinical risk.
Treatment OptionRisk LevelTypical Recovery TimeWhen RecommendedObservationLowOngoing monitoring; no recovery phaseAsymptomatic, no pathologyOrthodontic exposure + tractionModerateWeeks to months of orthodontic phaseImpacted canines with adequate spaceSurgical extraction (simple)Moderate3–7 daysPartially erupted or accessible impactionsSurgical extraction (complex / jaw surgery)Higher1–3 weeksDeeply impacted, proximity to nerves, or anatomic limitations
Bespoke Dental’s service offerings align with these clinical pathways: the practice provides extractions including wisdom tooth extraction, jaw surgery for complex impactions, and IV sedation for patient comfort during procedures. Advanced technology and experienced professionals enable safe surgical planning, and financing options through third-party providers are available for patients who require procedural care. Discussing these choices with a clinician allows you to match the treatment plan to your symptoms, imaging findings, and comfort preferences.
When Is Dental Extraction Recommended for Impacted Teeth?
Extraction is recommended when an impacted tooth causes pain, recurrent infection, cyst formation, damage to adjacent teeth, or when it obstructs orthodontic treatment goals. The decision considers impaction type—simple extractions may suffice for superficially impacted teeth, whereas deeply impacted or horizontally oriented teeth often require surgical bone removal and sectioning of the tooth for safe extraction. IV sedation is an option for anxious patients or complex procedures to improve comfort and cooperation. Postoperative recovery typically involves analgesics, soft diet, and follow-up to monitor healing and reduce complication risk.
What Are Alternative Treatments: Observation, Jaw Surgery, and Orthodontics?
Observation involves scheduled clinical and radiographic follow-up to ensure an asymptomatic impaction remains stable, avoiding unnecessary procedures for low-risk cases. Orthodontic exposure and traction collaborate between an oral surgeon and orthodontist to uncover an impacted anterior tooth and guide it into the arch using braces or attachments. Jaw surgery (orthognathic procedures) is reserved for severe anatomic restrictions where skeletal correction creates adequate space or resolves occlusal problems contributing to impaction. Combined care teams optimize outcomes by aligning surgical and orthodontic timing to restore function and aesthetics.
How Can You Manage Pain and Prevent Complications from Impacted Teeth?
Effective immediate management reduces symptoms and lowers the chance of complications while definitive care is planned, combining safe home measures with timely professional interventions when infection or severe pain occurs. Home strategies such as saltwater rinses, ice application, and over-the-counter analgesics can control inflammation and discomfort temporarily, while professional options include local anesthesia, prescription medications, drainage of abscesses, and IV sedation for procedural comfort. Preventive measures—orthodontic monitoring, timely removal of problematic third molars, and treatment of cysts—minimize long-term risks like bone loss or damage to adjacent teeth. Prompt recognition of worsening signs ensures early intervention and better outcomes.
Immediate home remedies for impacted tooth pain:
- Rinse with warm saltwater several times daily to reduce bacterial load.
- Apply a cold pack externally to reduce swelling and numb pain.
- Use over-the-counter anti-inflammatory analgesics per product instructions for pain control.
These home remedies can reduce symptoms but are not substitutes for professional evaluation when infection, persistent pain, or functional impairment is present.
Management ApproachApplicationExpected OutcomeSaltwater rinsesMultiple times dailyReduces surface bacteria and soothes mucosaCold packs10–15 minutes intermittentlyDecreases swelling and numbs superficial painProfessional antibioticsPrescribed for active infectionControls spreading infection pre-procedureIV sedation and in-office anesthesiaFor surgical proceduresImproves patient comfort and enables complex care
What Home Remedies and Professional Care Relieve Impacted Tooth Pain?
Effective short-term relief combines behavioral measures and targeted pharmacology: warm saline rinses reduce inflammation and help clear debris, cold packs limit swelling, and appropriate analgesics reduce pain enough to aid sleep and oral hygiene. When infection is present, clinicians may prescribe antibiotics or perform in-office drainage; these professional steps treat active infection and prepare the site for definitive extraction if needed. For patients anxious about surgery or facing complex extractions, IV sedation provides deeper relaxation and improved procedural tolerance. Coordinating home care with timely dental treatment prevents recurrent episodes and promotes predictable healing.
What Are the Risks of Untreated Impacted Teeth?
Leaving impacted teeth untreated can lead to recurrent pericoronitis, abscess formation, cyst or tumor development around the unerupted tooth, and progressive damage to adjacent teeth and bone, potentially requiring more extensive reconstruction. Chronic infection and cyst growth may cause resorption of neighboring roots and localized bone loss, complicating later extraction and increasing morbidity. Additionally, impacted anterior teeth left unmanaged can disrupt orthodontic alignment and facial esthetics. Recognizing these risks supports early assessment and appropriate intervention to limit long-term consequences.
After reviewing pain-management strategies, patients seeking evaluation or procedural care in the Lutz, FL area can consult Bespoke Dental for clinical assessment, radiographic imaging, and coordinated treatment planning. The practice’s expertise in wisdom teeth care and availability of IV sedation supports comfortable management of symptomatic impactions, and financing options can assist patients who require procedural care. Scheduling a consultation enables clinicians to match diagnostic findings with treatment options and to plan the safest, most effective path forward.